Women’s Health Topics
Updates from local experts
For this issue, we turn the spotlight on women’s health at every stage of life. From the greater impact of Alzheimer’s disease to the complexities of dense breast screening and the growing interest in complementary therapies for perimenopause, knowledge is power. These articles bring expert insights, practical guidance and a proactive path forward — helping women advocate for their bodies, their wellbeing and their futures.
Alzheimer’s Hits Women Twice as Hard
What to know about risk, caregiving and protecting brain health
Amba Kasongo, Programs Director
Alzheimer’s Association

As the number of people living with Alzheimer’s disease continues to rise across the country, its impact is felt unevenly among different groups. Women, in particular, face a double burden: they’re more likely both to develop Alzheimer’s disease and to care for someone living with the disease.
Consider a few facts: More than 12 million women in the United States live with or care for someone experiencing Alzheimer’s disease. Almost two-thirds of Americans living with the disease are women. And a woman’s estimated lifetime risk of developing the disease at age 65 is 1 in 5, compared to 1 in 10 for their male counterparts. What’s more, a 65-year-old woman is more than twice as likely to develop Alzheimer’s disease over the rest of her life as she is to develop breast cancer.
Why Are Women More at Risk?
Researchers are exploring several potential reasons why more women than men develop Alzheimer’s disease or other types of dementia. One of the most common explanations is that women tend to live longer and Alzheimer’s is more likely to develop as you age. However, age is likely not the only factor. New research is exploring whether risk is higher at any age and the role of other aspects such as biology, genetics or life experiences.
Another area of investigation is how women’s reproductive lives affect brain health across their lifespan. There have been studies, for example, that examine the risk of dementia and the age at first menstrual period, age at menopause, and time between first menstruation and menopause. While more research is needed, this study supports a promising theory — that events that happen across one’s lifespan, such as those associated with reproduction, may have an impact on dementia risk.
Researchers are also investigating sex-specific differences in the architecture of the brain. In a study released at the 2024 Alzheimer’s Association International Conference, scientists found that differences in the structural and functional connections of a woman’s brain may speed the spread of tau, a protein that’s a hallmark of Alzheimer’s disease. These findings could lead to new risk reduction strategies targeted for women.
Beyond biology, scientists believe that societal or cultural factors may also play a role in women’s risk. A recent study looked at work and family patterns, which have changed drastically over the last 100 years, and how these changes may play a role in a woman’s memory decline. The study indicated that women who participated in the paid labor force between early adulthood and middle age experienced slower memory decline in late life — building on previous research that links work and education with higher levels of cognitive engagement.
How Does Caregiving Impact Women’s Health?
When it comes to caregiving, there are inequities as well. More than 60% of Alzheimer’s and dementia caregivers are women — and more specifically, more than one-third are daughters. Women in the workforce are impacted as well, as nearly 19% of women dementia caregivers had to quit working either to become a caregiver or because their caregiving duties became too burdensome.
Studies have indicated that the overwhelming majority of dementia caregivers who request individual counseling and respite care are women. What’s more, women caregivers may experience higher levels of depression and impaired health than their male counterparts. Evidence suggests these differences arise because women caregivers tend to spend more time caregiving — to take on more tasks, and to care for someone with greater cognitive, functional or behavioral challenges.
How to Reduce Dementia Risk?
Research shows that people can reduce the risk of developing dementia by leading a healthy lifestyle. In 2025, a major breakthrough in brain health was announced at the Alzheimer’s International Association Conference. The U.S. POINTER Study, a two-year clinical trial involving more than 2,000 older adults, found that simultaneously targeting risk factors for cognitive decline — including regular physical activity, a brain-healthy diet, cognitive and social engagement, and health monitoring — can improve brain function in older adults.
The trial is the first of its kind to show that these interventions work across diverse communities, regardless of age, gender or genetic risk. The results provide powerful, actionable guidance for promoting brain health. Specifically, the U.S. POINTER brain health recipe includes:
- Physical exercise — 30–35 minutes of moderate-to-intense aerobic activity four times a week, plus strength and flexibility exercises twice a week.
- Cognitive exercise — Computer-based brain training three times a week for 30 minutes, plus regular engagement in intellectually challenging and social activities.
- Nutrition — Adherence to the MIND diet, which emphasizes dark leafy greens, berries, nuts, whole grains, olive oil and fish, and which limits sugar and unhealthy fats.
- Health monitoring — Regular check-ins on blood pressure, weight and lab results.
Women can take charge of their brain health by incorporating these and other healthy habits such as not smoking, maintaining a healthy weight and managing diabetes. The Alzheimer’s Association also provides tools, like the Brain Health Habit Builder tool, available online and which can be used to check current habits — such as physical activity, diet and sleep — and make a plan to protect the brain.
More research is needed, and with more understanding will come new tools and best practices for addressing risk, prevention, detection and additional dementia treatments. Until then, women can take heart in adopting the positive actions that have been proven to make a real difference in brain health.
And all women are encouraged to access the resources provided by the Alzheimer’s Association, which include disease education and help for caregivers — such as support groups and navigation tools — all of which are accessible through the Alzheimer’s Association 24/7 Helpline (800-272-3900).
 With more than a decade of nonprofit and public health experience, Amba Kasongo is Programs Director for the Alzheimer’s Association. She leads a team that conducts education and training, empowers volunteers, and develops and nurtures corporate and community partnerships for the Association, which is the world’s leading voluntary health organization in Alzheimer’s care, support and research. ALZ.org
With more than a decade of nonprofit and public health experience, Amba Kasongo is Programs Director for the Alzheimer’s Association. She leads a team that conducts education and training, empowers volunteers, and develops and nurtures corporate and community partnerships for the Association, which is the world’s leading voluntary health organization in Alzheimer’s care, support and research. ALZ.org
Breast Density
What every woman should know about her mammogram
Angela Jain, MD
Fox Chase Cancer Center
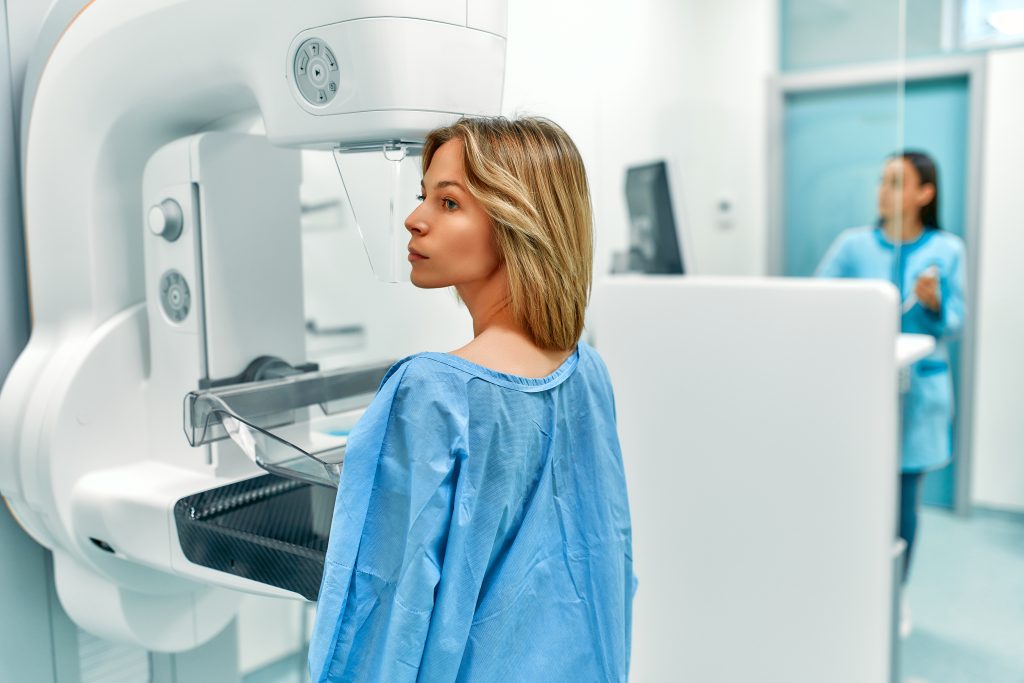
For many women, a mammogram is a familiar part of routine health care — something checked off the calendar every year or two with little fanfare. But for millions of women, the results of that mammogram may include a term that raises new questions and concerns: dense breasts.
What does breast density mean? Why does it matter? And how should it affect decisions about breast cancer screening?
Understanding breast density can empower women to have more informed conversations with their health care providers and to take an active role in their breast health.
What Is Breast Density?
Breast density refers to the composition of breast tissue, not how the breasts feel to the touch. On a mammogram, breast tissue appears in shades of black and white. Fatty tissue looks dark, while glandular and connective tissue — known as fibroglandular tissue — appears white.
Breasts are considered “dense” when there’s more fibroglandular tissue than fatty tissue. Radiologists classify breast density into four categories: 1. almost entirely fatty, 2. scattered areas of fibroglandular density, 3. heterogeneously dense and 4. extremely dense.
Women in the last two categories are considered to have dense breasts. This is very common — about half of women who undergo mammography fall into one of these dense categories.
Why Does Breast Density Matter?
Breast density is important for two key reasons. First, dense tissue can hide cancer. Because both dense tissue and tumors appear white on a mammogram, cancers can be harder to see in dense breasts. This is sometimes described as trying to find a snowball in a snowstorm. As a result, mammograms may be less sensitive in women with dense breasts.
Second, dense breasts are a risk factor. Having dense breasts slightly increases a woman’s risk of developing breast cancer. While density alone does not mean cancer will develop, it is considered one of many risk factors, along with age, family history, genetic mutations, personal health history and lifestyle factors.
How to Know If You Have Dense Breasts
Breast density can’t be determined by a physical exam or breast size. The only way to know is through a mammogram. After your screening, the radiologist evaluates the images and assigns a density category.
In many states — and now under federal regulations — women are notified if they have dense breasts as part of their mammogram results. This notification is meant to encourage discussion between patients and their health care providers, not to cause alarm.
Does Breast Density Change Over Time?
Yes. Breast density can change throughout a woman’s life. Density often decreases with age, particularly after menopause, but this is not always the case. Hormone replacement therapy may increase or maintain breast density, while other factors such as weight changes or medications may influence it as well.
Because breast density can change, it’s evaluated each time a mammogram is performed.
Is Mammography Still Important With Dense Breasts?
Absolutely. Mammography remains the most effective screening tool for reducing breast cancer deaths and is recommended for women of average risk starting at age 40, or earlier for some women at higher risk.
Even though dense tissue can make interpretation more challenging, mammograms still detect many cancers in dense breasts. Newer technologies, such as digital breast tomosynthesis (3D mammography), have improved cancer detection and reduced false positives, especially in women with dense tissue.
Are Additional Screening Tests Needed?
For some women with dense breasts, supplemental screening may be recommended. This decision is individualized and based on overall breast cancer risk, not density alone.
Possible additional screening options include: breast ultrasound, which can detect cancers that may not be visible on mammography, and breast MRI, typically recommended for women at high risk due to genetics or strong family history.
While these tests may find additional cancers, they can also increase the likelihood of false positives, leading to extra imaging or biopsies that turn out to be benign. For this reason, the benefits and risks should be carefully weighed in consultation with a health care provider.
What to Know About Breast Cancer Risk
Breast density is just one piece of the cancer risk puzzle. Many women with dense breasts never develop breast cancer, and many women with breast cancer do not have dense breasts.
Your provider may use a risk assessment tool that considers multiple factors, such as age, family history of breast or ovarian cancer, personal history of breast conditions, genetic test results and reproductive history.
This broader view helps guide screening recommendations that are tailored to you.
What Can You Do as a Patient?
Knowledge is power when it comes to breast health. If you’ve been told you have dense breasts, consider taking the following steps:
- Ask questions about your mammogram report and what your density means for you.
- Discuss your personal risk for breast cancer with your health care provider.
- Review screening options, including the potential benefits and drawbacks of supplemental tests.
- Stay up to date with recommended screenings.
- Report any breast changes — such as lumps, pain, nipple discharge or skin changes — promptly, regardless of recent imaging.
Breast awareness and regular screening work together to support early detection.
A Reassuring Perspective
Hearing that you have dense breasts can feel unsettling, but it’s important to remember that density is common and manageable. It’s not a diagnosis, and it doesn’t mean something is wrong.
Advances in imaging, increased awareness and personalized screening strategies have made it possible to detect breast cancer earlier and more accurately than ever before. Open communication between patients and health care providers is the cornerstone of this progress.
Breast density is a normal and important part of breast health. Understanding what it means — and what it doesn’t mean — can help women make informed decisions without unnecessary fear.
If you have dense breasts, you’re not alone. With the right information, appropriate screening and ongoing dialogue with your care team, you can take confident steps to protect your health.
 Angela Jain, MD, Chief of the Division of Gynecologic Medical Oncology at Fox Chase Cancer Center and Associate Professor in the Department of Hematology/Oncology, specializes in the treatment of gynecologic cancers and breast cancer. In addition to her clinical work, her research focuses on clinical trials to improve outcomes and treatment options in women’s cancers and retrospective outcomes-based research, focusing on improving the quality, effectiveness and value of cancer care. FoxChase.org
Angela Jain, MD, Chief of the Division of Gynecologic Medical Oncology at Fox Chase Cancer Center and Associate Professor in the Department of Hematology/Oncology, specializes in the treatment of gynecologic cancers and breast cancer. In addition to her clinical work, her research focuses on clinical trials to improve outcomes and treatment options in women’s cancers and retrospective outcomes-based research, focusing on improving the quality, effectiveness and value of cancer care. FoxChase.org
Nurturing Yourself Through Perimenopause: A Holistic Path to Well-Being
With tips for women of all ages
Beverly Fornoff
Penn Medicine
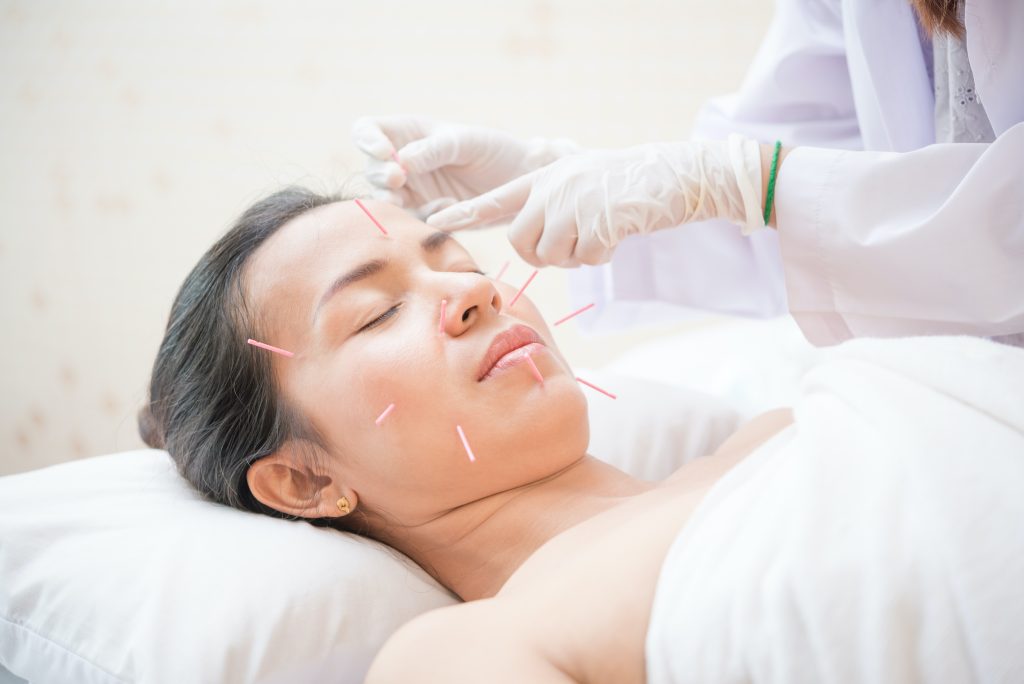
Perimenopause can be a challenging time for many women, especially if they’ve spent a lifetime caring for others. This caretaking often occurs at the expense of nurturing their own health.
By the time many women notice shifts associated with approaching menopause, they may feel the need to step away from putting out fires for others and begin tending to their own blazing infernos. Taking some time to quietly look within and prioritize their own health needs might feel impossible or even selfish, but it’s the most important step they can take to be able to continue caring for their families, careers and other responsibilities.
At this phase of their lives, some women are turning to complementary medicine for support in managing the stress of midlife demands and their changing health needs. Acupuncture and Chinese herbal medicine are just two options that are becoming mainstream modalities and increasingly accepted and used alongside conventional Western medicine, often within existing health organizations.
Acupuncture and How it Helps
Acupuncture involves inserting sterile, fine needles in specific points on the body. The needles evoke a response from the nervous system, sending messages to the brain that stimulate neurochemicals affecting pain, hormonal balance, blood quality and circulation, and mood, among other things. Studies have shown that acupuncture is effective at reducing hot flashes, sleep disturbances, depression, anxiety and perceived stress — all symptoms commonly associated with perimenopause.
Treatment strategies may include acupuncture point combinations that would cool the heat and improve fluid metabolism toreduce hot flashes and night sweats, supplement energy production to reduce fatigue and improve brain function, and regulate the nervous system to improve sleep and reduce anxiety and depression.
As few as four needles or as many as 20 or more may be used in a session. Needles are generally retained in place for 20 to 30 minutes while the patient relaxes before being removed. Each acupuncture session also includes time to discuss symptoms and treatment strategy, lasting about an hour in total.
Treatment frequency is based on each woman’s needs, and most commonly begins with weekly sessions, gradually decreasing as symptoms improve. Some women choose to continue maintenance treatment, while others stop once their symptoms are under control.
Chinese Herbal Medicine
Chinese medicine includes more than acupuncture. Herbal medicine can also be used to balance menopausal symptoms. Herbal formulas may be prescribed by a licensed acupuncturist who also holds a certificate in Chinese herbs, meaning they’ve completed two years of herbal study and passed a national board exam.
Chinese herbs are rarely prescribed as a single ingredient. Most often formulas are combinations of herbs that complement one another. Herbal formulas can be taken as raw herbs, granular tea or in capsule form. They may also be prepared as a tincture or poultice.
In perimenopause, herbs can be used to reduce hot flashes, regulate the menstrual cycle, improve sleep and support the nervous system. This approach helps reduce the effects of stress with similar strategies and diagnostic process as with acupuncture.
There’s no “one size fits all” herbal prescription. Each formula is custom designed to fit the patient’s specific symptoms. Practitioners of Chinese medicine also view food as medicine and often provide dietary recommendations based on the energetic properties of foods and a person’s diagnostic symptoms.
More Holistic Care Therapies
During times of high stress, it’s important to maintain physical movement to keep the joints healthy and the muscles flexible. Yoga, tai chi and qi gong are all gentle movement exercises that improve flexibility, strength and balance without causing strain or increasing inflammation.
Yoga focuses on flexibility and body awareness and can be easily modified by a trained instructor to accommodate physical limitations. Tai chi, while initially designed for self-defense, has evolved into a slow-moving exercise that can strengthen muscles and joints as it improves focus and balance. Qi gong combines slow movement and awareness of breathing to cultivate qi (vital energy).
Mental well-being is also important to address. Meditation fosters mindfulness by teaching individuals to observe their thoughts without becoming caught up in the story and drama. This practice can increase positive feelings toward themselves and others, allowing better coping with worry and stress that are so common at this stage of life. Studies show that many types of meditation — such as Mindfulness-Based Stress Reduction, Loving–Kindness and Compassion Meditation, and Focused Attention (such as on the breath) — can affect the length of telomeres on a gene strand, an indicator of slower aging.
Massage is another self-care tool that can reduce muscle aches and pain through physical manipulation of the fascia, muscles, tendons and ligaments. Benefits can be achieved in as little as 15-to-20-minute sessions for those who may have trouble fitting a longer 60-minute session into a busy schedule. Massage can also promote relaxation, as appropriate professional touch can increase endorphins and reduce cortisol.
More options include sound and vibration, which have been used for many years for their health benefits and have recently gained popularity for their ability to calm the nervous system. The use of gongs, singing bowls and tuning forks among other instruments have all been used for their ability to produce sound waves that resonate through the body to stimulate relaxation and support a balanced nervous system through vagal nerve activation. This type of therapy can be experienced in private or group sound immersion sessions and can be experienced sitting in a chair or lying on the floor or a table.
How to Choose
Many primary care physicians understand the benefits and strengths of complementary modalities and may be able to refer you to a practitioner. A well-trained, licensed acupuncturist has expertise in most of the modalities mentioned here or has a network of practitioners to refer you to.
It’s important to know about the training, licenses and certifications of your practitioner, as levels of education can vary. And it’s important to feel comfortable and have rapport with your practitioner, so feel free to ask questions during your consultation.
An increasing number of women are seeking complementary therapies in addition to Western care as they navigate their journey through perimenopausal challenges. With proper support, this can also be a magical time of self-empowerment as women begin to make room for themselves and their own health.
 Beverly Fornoff, MAc, is a licensed acupuncturist at the Women’s Specialty Center at Penn Medicine Lancaster General Health Holistic Therapy. She received her graduate degree from Maryland University of Integrative Health and has been in practice for more than 23 years. For more information on holistic therapy and perimenopausal care, visit PennMedicine.org.
Beverly Fornoff, MAc, is a licensed acupuncturist at the Women’s Specialty Center at Penn Medicine Lancaster General Health Holistic Therapy. She received her graduate degree from Maryland University of Integrative Health and has been in practice for more than 23 years. For more information on holistic therapy and perimenopausal care, visit PennMedicine.org.
